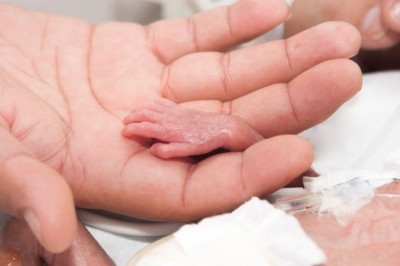
Premature babies’ gut health may benefit from probiotic-boosted milk, study finds

Researchers suggest the routine use of Lactobacillus and Bifidobacterium probiotics have a preventative effect on necrotising enterocolitis (NEC) and late-onset sepsis, in preterm neonates.
The team say a lack of safety issues observed in the study corresponds to no published reports on the safety or efficacy of routine probiotics used in any UK centres.
“Ours is the first UK study to evaluate the potential impact of routine probiotics use on NEC and sepsis rates,” says Dr Paul Clarke, study team member and Norwich University Hospital (NNUH) consultant neonatologist
“It has been a big team effort to boost the gut health of these tiny vulnerable babies at the beginning of their lives and help them get the right gut bacteria from the start,” says Dr Clarke, also an honorary professor at University of East Anglia (UEA).
Necrotising enterocolitis (NEC) is a condition in which a part of the bowel dies. It typically occurs in premature newborns that are of low birthweight (below 1500 grams (g)).
Abnormal gut microbiota is recognised as central to NEC and observational studies have shown that prophylactic probiotics prevent NEC in preterm babies.
Currently, UK centres do not use probiotics routinely due to questions about effectiveness. Previous trials do not show benefit, probiotic dosage, treatment duration and NEC definitions to assess efficacy.
Study details
The team from NNUH, UEA and the Quadram Institute began reviewing the outcomes of around 1,000 premature babies admitted to the NNUH’s Neonatal Intensive Care Unit (NICU) over a 10 year period from 1 January 2008 to 31 December 2017.
Prior to 1 January 2013 probiotics were not used. After this date, dual-species Lactobacillus acidophilus and Bifidobacterium bifidum combination probiotics were routinely administered daily to high-risk neonates.
As of April 2016, triple-species probiotics (L.acidophilus, B.bifidum, and B.longum subspecies infantis) were used.
The team found that rates of NEC fell from 7.5% (35/469 neonates) in the pre-implementation period to 3.1% (16/513 neonates) in the routine probiotics period.
The more than halving of NEC rates after probiotics introduction was independent of other factors including breast milk feeding rates.
Meanwhile, cases of late-onset sepsis fell from 106/469 (22.6%) to 59/513 (11.5%) and there was no episode of sepsis due to Lactobacillus or Bifidobacterium.
All-cause mortality also fell in the routine probiotics period, from 67/469 (14.3%) to 47/513 (9.2%), although this was not statistically significant after multivariable adjustment.
“This work highlights how modulating the preterm gut microbiota with beneficial bacteria like Bifidobacterium can result in real improvements in health outcomes in these fragile and at-risk babies,” says Dr Lindsay Hall, study team member and Microbiome Research Leader at the Quadram Institute Bioscience (QIB).
“The next stage is to understand how this type of supplementation modulates the wider microbial community and the mechanisms behind these beneficial effects.”
Further research needed
The team note that probiotic impact appeared greatest in the first two weeks after birth, suggesting that aiming for very early postnatal probiotic bacterial gut colonisation was crucial.
They also pointed out their findings only support an association and cannot conclusively determine that probiotics caused the observed markedly reduced NEC incidence.
“It is critical to note that there are significant differences between individual Bifidobacterium and Lactobacillus species and also huge strain variability, not least in ability to digest dietary components such as HMOs and in their immune and infection modulatory traits,” the study highlights.
“Further studies are needed to determine the generalisability of the underlying potential benefits of multispecies probiotics in this at-risk cohort.”
The rapidly evolving universe of probiotics, prebiotics and the microbiome will be discussed in-depth at the upcoming Probiota 2020 in Dublin on February 10-12.
From microbiome advances, to start-up game changers, market stats, crucial clinical science and regulatory knowledge, this is a congressional must-have.
Will you be joining your peers in one of Europe’s greatest cities?
Source: Archives of Disease in Childhood – Fetal and Neonatal Edition
Published online: doi: 10.1136/archdischild-2019-317346
“Incidence of necrotising enterocolitis before and after introducing routine prophylactic Lactobacillus and Bifidobacterium probiotics.”
Authors: Claire Robertson, George M Savva, Raducu Clapuci, Jacqueline Jones, Hassan Maimouni, Eleanor Brown, Ashish Minocha, Lindsay J Hall, Paul Clarke.