Faecal transplants show potential in reducing alcoholism, study suggests

The researchers point to FMTs containing the bacteria Lachnospiraceae and Ruminococcaceae as beneficial in patients diagnosed with alcohol-use disorder (AUD) and were suffering from alcohol-related cirrhosis of the liver.
Patients receiving the transplant had a reduced appetite and had notably fewer alcohol-related metabolites in their urine. After six months, those treated with FMT exhibited fewer AUD-related behaviours.
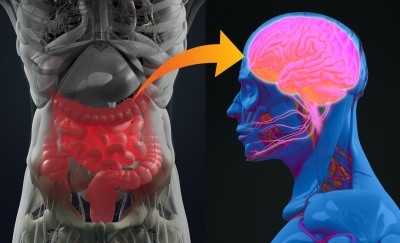
“The way to the brain is through the gut,” says Dr Jasmohan Bajaj, lead study author and a professor based at the Virginia Commonwealth University (VCU) school of medicine. “This research is preliminary but could be a glimmer of hope for people living with addiction diseases.”
“People with alcohol use disorder are often discriminated against and given up on,” he adds. “But it’s a disease like any other. There’s a genetic predisposition, and addictions may be promoted by those gut microbes.”
Gut-brain axis link?
AUD has previously been linked to changes in the gut-brain axis made worse by the manifestation of cirrhosis.
Previous studies have identified a potential role of microbiota in addictive behaviour as well as the altered gut-brain axis response to an FMT.
While abstinence from alcohol is linked with microbial change, the impact of microbial modulation to assist in the reduction of alcohol misuse remains unclear.
Writing in the journal Hepatology, the research team began gathering the transplanted faecal material from a single donor.
Analysis revealed this stool was rich with two specific bacteria, Lachnospiraceae and Ruminococcaceae, which were missing in the stool of the 20 men with AUD-related cirrhosis.
This sample received the transplant via enema, and a random half of them received a placebo. They all returned interviews and tests as part of the follow-up procedure.
Results revealed nine of the ten patients receiving the transplant exhibited a reduction in their cravings and a reduction in the urine measurement of alcohol-related metabolites.
Along with a reduction in their drinking, the men who received the transplant also described an improved quality of life with cognitive analysis verifying an improvement in inhibitory control. In contrast, only three of the placebo participants saw improvements.
‘Larger trials needed’
“While the mechanism of this longer-term change is unclear, the lower event rate in FMT-assigned patients could reflect the reduction but not the absence of alcohol intake in more patients in the FMT versus placebo group,” the team writes.
“These findings are in line with prior long-term studies of FMT in hepatic encephalopathy and alcoholic hepatitis and extend these into patients with AUD.
“However, since this is a phase 1 study, larger trials are needed to extend these findings.”
Dr Peter Buckley interim CEO of VCU Health System, interim senior vice president of VCU Health Sciences and dean of the School of Medicine adds, “Dr Bajaj’s research into addiction is incredibly important and timely, and I’m excited to see what comes of expanded trials in future phases.
“At VCU, we’ve been tireless in the pursuit of better health outcomes for our patients — and patients everywhere.”
Source: Hepatology
Published online: doi.org/10.1002/hep.31496
“A Randomized Clinical Trial of Faecal Microbiota Transplant for Alcohol Use Disorder”
Authors: Jasmohan Bajaj et al