As part of the Newcastle 85+ cohort Study, researchers from Newcastle University in the UK tracked the eating habits of 793 85-year-olds (302 men and 491 women) using two non-consecutive 24-hour recalls conducted by trained research nurses.
They found energy and non-starch polysaccharide (NSP) intakes were far lower than that recommended for this group in the UK.
Only 20% of the participants had higher energy intakes than the estimated average requirement (EAR) set.
Meanwhile intakes of NSP – a major part of dietary fibre – were also very low and saturated fatty acid (SFA) intakes very high compared to dietary reference values (DRV).
“Although the low NSP intake is likely to contribute to the high prevalence of constipation in very old people, the health significance of the relatively high SFA intake in this age group is unknown,” they wrote in the British Journal of Nutrition.
“In general, the lack of robustly based dietary recommendations for very old people limits our ability to interpret the dietary intakes of the Newcastle 85+ Study participants by reference to age-appropriate DRV.
“It is essential that the very old are included in future nutrition studies to inform the development of new, age-specific DRV.”
They said the results highlighted the “paucity of data” on dietary intake and the uncertainties about DRV for this age group.
A neglected population
In this study the researchers compared intakes against current UK DRVs.
Yet apart from the EAR for energy intake and the reference nutrient intake for protein, which sets a DRV for those aged 75 years and over and 50 years and over, respectively, all other UK DRVs lump everyone aged 18 years and over into the same category.
Research also neglected this older population.
"Many studies arbitrarily exclude very old people for no reason other than age, while others only include a small number, resulting in a lack of statistical power. For example, a Europewide, multi-centre study on food intake in older adults (Survey Europe on Nutrition in the Elderly: A Concerted Action) had an upper age limit of 79 years."
Fastest growing age segment in the West
The steady rise in life expectancy and decrease in later-life mortality make very old people – those aged 85 years and over – the fastest growing age segment of Western societies.
In the UK, there are now more than 1.5 million over 85s – that’s 2.5% of the total population. This figure is set to rise to 3.3 million or 5% over the next 20 years.
Meanwhile reduced mobility, financial constraints, disease and taste perception means this group is particularly vulnerable to deficiencies and malnutrition.
In the UK, over 10% of those aged 65 years and over and 18% of over 85s are at medium or high risk of malnutrition, of which unintended weight-loss is a key signpost.
In this latest study the researchers said the failure of the majority of participants to meet current energy EAR might lead to unintended weight-loss.
This carries a huge public health price tag, with public expenditure on disease-related malnutrition estimated to exceed £13 billion (€16.44bn) per year in the UK alone, with over half of this relating to over 65s.
Despite these significant figures, very little is known about the dietary habits of this age group.
Impaired cognition was one challenge faced when recording the diets of this age group, which can lead to misreporting, they said.
The findings
The median energy intake was 6.65 megajoules (MJ) per day – 46.8% of which was from carbohydrates, 36.8% from fats and 15.7% from proteins.
This was much lower than the estimated average requirements for energy of 9.6 MJ per day for men and 7.7 MJ per day for women.
Average NSP intake was 10.2 g per day but this was higher in non-institutionalised, more educated, more physically active 85-year-olds from a higher social class.
Again this average was lower than the DRV of at least 18 g per day.
The median SFA intake was higher than the DRV.
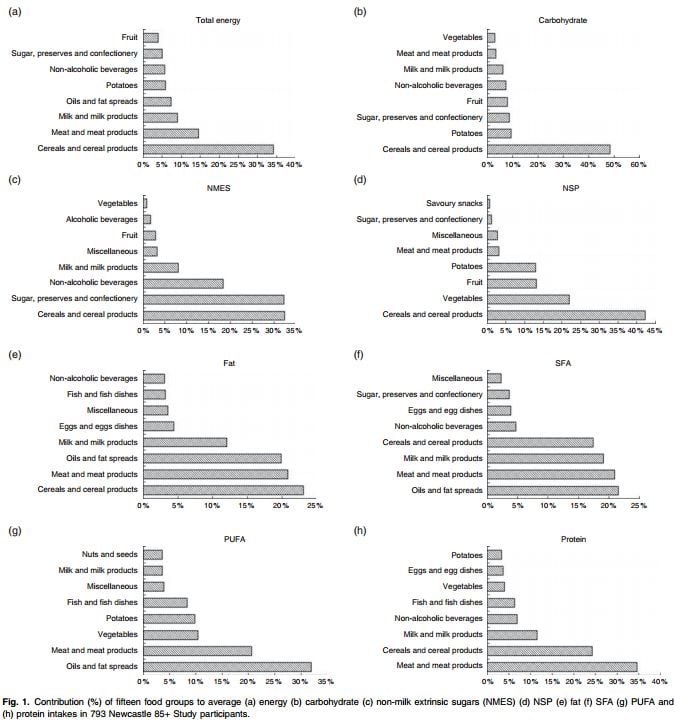
Cereals and cereal products were the top contributors to intakes of energy and most macronutrients (carbohydrates, non-milk extrinsic sugars, NSP and fat), followed by meat and meat products.
The researchers also collected data on the use of laxatives within this cohort, which will be explored in a future paper.
Source: British Journal of Nutrition
Published online ahead of print, doi:10.1017/S0007114516001379
“Macronutrient intake and food sources in the very old: analysis of the Newcastle 85+ Study”
Authors:N. Mendonça et al
