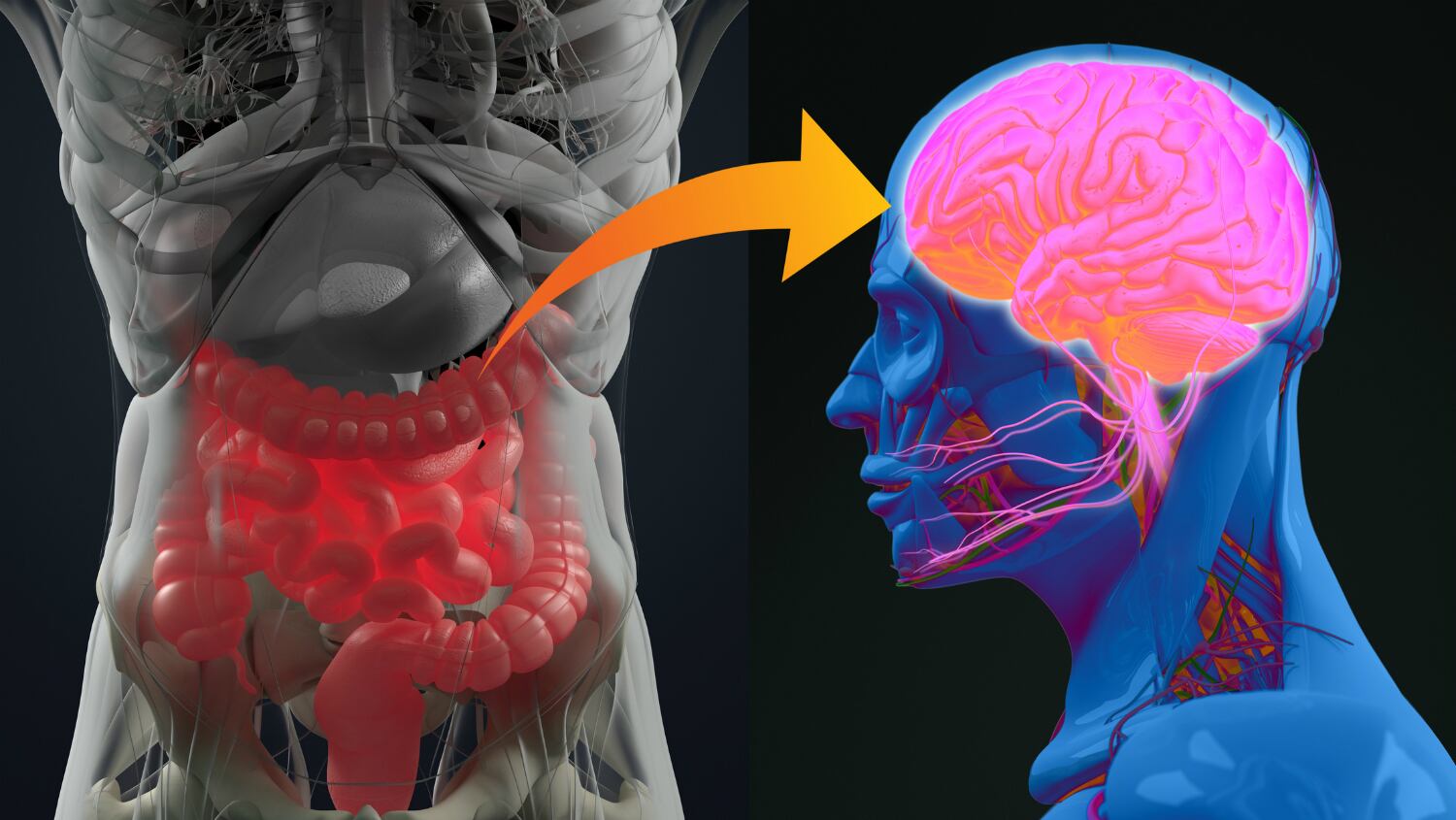
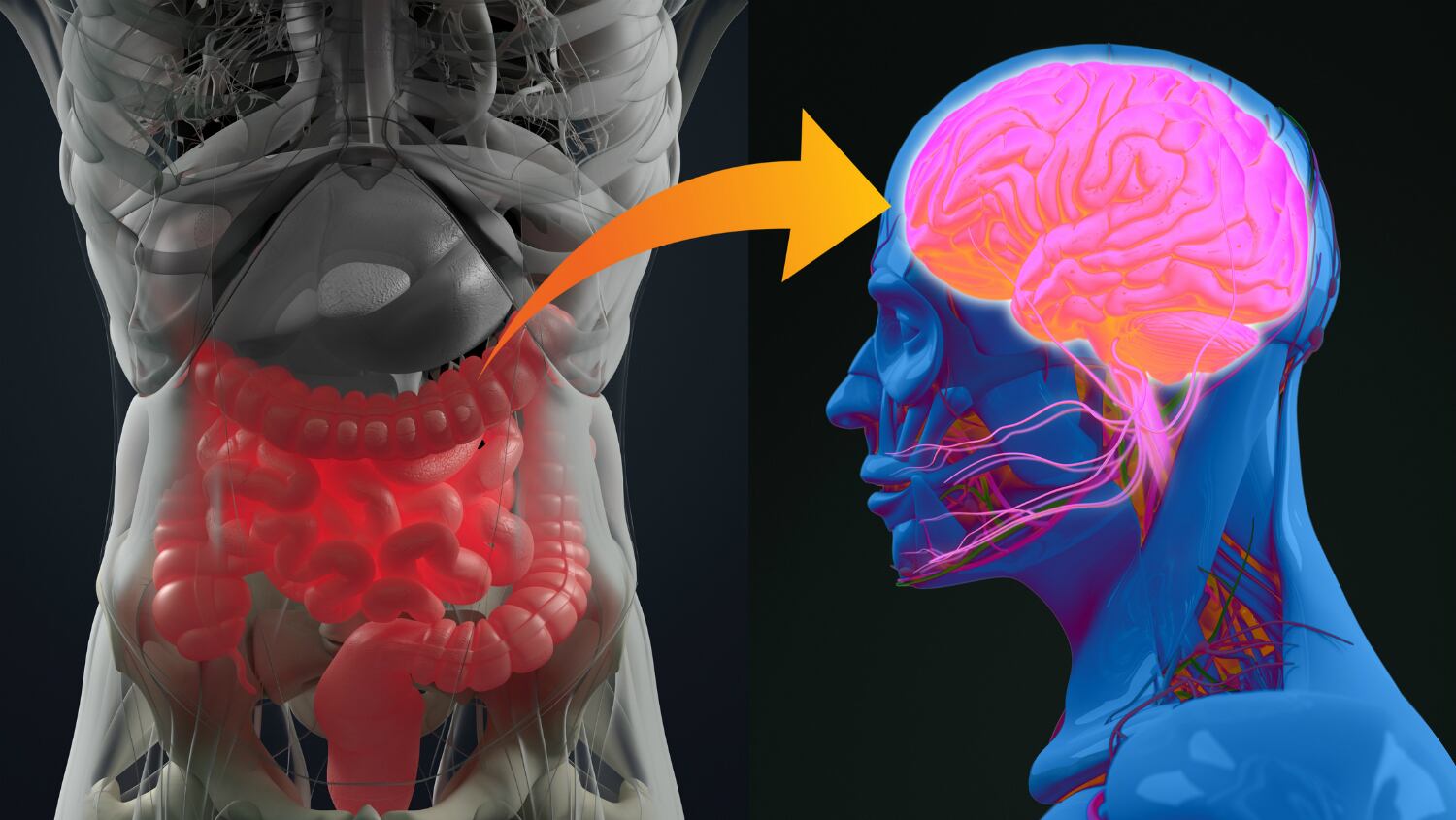
The first two to three years of life are when the gut microbiota of infants grows in diversity and richness. It is understood that disruptions in the evolving gut microbiota during such a critical period can affect cognitive development, which can in turn lead to complications that last well into adulthood.
While scientists have determined that communication between the microbiota, gut and brain is driven by neural and hormonal regulation, as well as metabolic and immune pathways, the underlying parallel developments of this communication are still unclear.
Based on this, the researchers reviewed the known associations between gut microbiota and brain development and function in early life, assessed the potential mechanisms involved, and reported on how nutritional intervention could further modulate the microbiota and, by extension, cognitive function and development.
Developmental parallels
The review noted developmental parallels between the gut in brain in early life, stating that "many factors known to influence the development of the gut microbiota, such as gestational age and mode of feeding, e.g., breast feeding versus formula, are thought to affect brain development and function".
However, it also said it was difficult to determine if the effects on brain development was mediated through nutrients directly impacting the brain, or of some of them were the result of nutrients acting on the gut microbiota, which then influences brain development and function.
The researchers also proposed three possible mechanisms to explain how gut microbiota may communicate with the brain.
Blood-brain barrier regulation
The first suggested mechanism was the gut microbiota's regulation of the blood-brain barrier, gut glial cell homeostasis, and microglia maturation.
The blood-brain barrier is known to play a vital role in brain development by protecting the brain from external harm. Hence, a highly permeable blood-brain barrier is considered less protective, making the brain more susceptible to pro-inflammatory cytokines, glucocorticoids, and bacterial metabolites, all of which can inhibit regular, healthy brain development.
An earlier mouse study found that colonisation of the gut during young adulthood — when the barrier is highly permeable — improved the barrier's integrity within two weeks.
Other rodent studies have reported that, like the blood-brain barrier, the gut epithelial barrier can also be modulated by the gut microbiota, with its permeability regulated by gut mucosal glial cells.
This suggests that the gut microbiota may regulate gut barrier integrity — at least partially — through these glial cells.
There was also evidence that the gut microbiota may act through enteric glial cells, with a recent mouse study showing that gut mucosa development by glial cells starts in early postnatal life, reaching steady-state levels after weaning.
However, this was observed only in mice with gut microbiota and not germ-free mice, which lacked gut mucosal glial cells and exhibited global defects in brain microglia.
The researchers added that the gut microbiota may also support gut-brain communication and drive the maturation and function of gut glial cells, though this association is not yet fully understood.
They also hypothesised that the gut microbiota may influence brain development by regulating the blood-brain barrier.
The HPA axis
The second suggested mechanism was the gut microbiota's activity via the HPA (hypothalamic-pituitary-adrenal) axis, which encompasses a set of interactions between two parts of the brain — the hypothalamus and pituitary glands — and the adrenal glands situated at the top of the kidneys.
This axis is crucial in the regulation of digestion, immune function, mood, emotional responses, and energy storage and expenditure. Microbial colonisation in early life is necessary for the axis to develop normally.
Early-life stress has been shown to increase plasma corticosterone in rat pups, which indicates higher HPA axis activity and is linked to greater intestinal permeability.
The researchers wrote that in a 'circular relationship', the HPA axis would be able to regulate the immune system, gut permeability, and gut microbiota colonisation / composition, and vice versa.
They added: "These findings indicate that colonisation of gut microbiota in early life plays a critical role in the regulation of HPA responses, and environmental challenges that generate stress could translate into changes in microbiota colonisation and composition via HPA axis modulation.
"Colonisation by either beneficial (e.g., bifidobacteria) or pathogenic (e.g., enterobacteria, enterococci, Escheria coli) gut microbiota can direct the HPA in opposing directions, with either positive or negative consequences for the host."
Additionally, the vagus nerve system plays an important part in maintaining HPA axis homeostasis, and affects gut-brain communication — in fact, variations in early-life gut microbiota colonisation influences vagus nerve responses differently.
However, this requires more thorough studies that use distinct microbial interventions in early life, so researchers can understand the nature of the signals transmitted to the brain.
Bacterial metabolite production
The third suggested mechanism was the production of bacterial metabolites, such as short-chain fatty acids (SCFAs) and neurotransmitters, such as serotonin, dopamine, and γaminobutyric acid (GABA).
Proper brain development and function requires a balance between inhibitory (GABA) and excitatory (glutamate) neurotransmitters. For instance, insufficient GABA alongside excessive glutamate is associated with autism spectrum disorder and ADHD.
Currently, any relative contribution from bacterial production of neuroactive compounds to this balance is unclear, with certain SCFAs able to partially cross the blood-brain barrier and affect its permeability and directly affect learning and memory.
The researchers stated that it was thus "plausible to hypothesise (that) SCFAs produced in the colon by gut microbiota could impact learning and memory through chromatin remodelling".
However, the physiological levels of SCFAs necessary to support healthy brain development at different early-life stages are still unclear.
At the same time, the gut microbiota is said to be crucial to the metabolism of tryptophan, the precursor of serotonin, which is actively involved in postnatal establishment and refinement of brain wiring.
Roughly 90% of the body's serotonin is synthesised in the digestive tract, mainly by enterochromaffin cells that regulate gut-brain communication.
Although serotonin synthesised in the periphery cannot cross the blood-brain barrier, the gut microbiota is thought to control serotonin in the brain via tryptophan regulation, with a recent study showing that indigenous spore-forming gut bacteria can modulate tryptophan metabolism, as well as serotonin production.
The researchers concluded: "The concept of a microbiota gut-brain axis is a relatively new concept that has evolved over the past decade. Much of our knowledge on the relationship comes from pre-clinical studies; carefully controlled clinical studies are necessary in order to understand the translational strength of these findings.
"Early-life nutrition is an important modifiable factor that can shape both gut microbiota and brain development. We have little understanding of the longer-term programming effects of the interaction between the gut microbiota and brain development during early life and how these may affect susceptibility to later challenges.
"Thus, hype aside, understanding the complexity of this relationship may well revolutionise our understanding of brain development, understand specific windows of opportunity instrumental to a healthy development of gut-brain communication, and uncover novel nutritional ingredients that via these routes promote and protect normal brain development, and reduce the risk on neurodevelopmental and neuropsychiatric disorders in early life."
Source: Neuroscience and Biobehavioral Reviews
https://doi.org/10.1016/j.neubiorev.2018.09.002
"Targeting the gut microbiota to influence brain development and function in early life"
Authors: Shugui Wang, et al.