Study attempts to answer if gut bacteria plays rheumatoid arthritis role
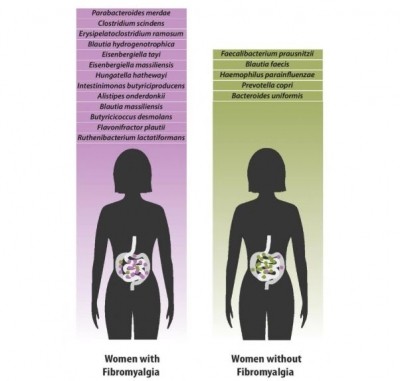
The team identifies bacteria from the Prevotella group as a potential trigger for the early stages of RA, a condition that affects around 29 cases/100,000 in northern Europe and 16.5/100,000 in southern Europe.
“Our findings are in agreement with the gut microbiome having a role in the development of RA,” says first study author Philippa Wells a researcher at the department of twin research and genetic epidemiology at King's College London.
“Speculatively, in the future this could be a possible target for treating the condition. This is something future studies will need to explore.”
RA has a substantial genetic component, with heritability estimated at 65%. One RA risk factor is the mucosal commensal microbiota, where extensive crosstalk exists between microbiota and the host.
This communication starts early in life with the development of a normal immune system. The gut lumen holds most of the commensal microbiota and is located close to the immune system and the systemic circulation.
Prevotella copri increase
A key gut microbiota association in patients with RA is a relative increase in the abundance of Prevotella spp, particularly Prevotella copri (P copri), which presents early in RA.
While P copri is linked to promoting RA activity, the gut microbiota may also influence the response to treatment of patients with the condition.
Along with colleagues from the university of Geneva and Hannover medical school, the team began looking at the genetic and microbiome data of 1,650 TwinsUK participants with no history of RA.
This is so that they could see if they could spot any early warning signs before the onset of symptoms.
The team also calculated the twins’ genetic risk for RA and then looked at the gut bacteria identified from stool samples.
The researchers found the presence of Prevotella spp were positively associated with RA as well as an association between the group and the presence of preclinical RA phases, discovered when the team analysed data from participants in another cohort study.
“By understanding how specific bacteria in the gut affect the development of RA we not only open the door to more targeted, effective treatments, but we can begin to tackle the disease sooner,” says Natalie Carter, head of research engagement at Versus Arthritis, which funded the study.
“Implementing treatment that works as early as possible will keep joint damage to a minimum, help people manage their condition and allow them to lead full and active lives.”
Findings’ importance
In discussing the findings’ significance, the team highlights work identifying P copri’s link to new-onset RA before treatment with disease-modifying antirheumatic drugs, as well as an association with other inflammatory conditions,
This, they say fuels speculation that inflammation is a prerequisite for P copri proliferation within the gut, relative to other taxa.
“P copri might have adapted to thrive in a pro-inflammatory environment, and might further promote the inflammatory milieu, thereby enhancing the bacteria's own favoured environmental niche,” the team writes. “In doing so, P copri may contribute to RA pathology.”
Further theory centres around the suggestion the microbiota is altered before disease. Indeed, the team found similar results in the patients with preclinical RA in first-degree relatives of patients with RA.
“Our follow-up investigation of patients with pre-RA revealed a further six novel genus associations, which had not been evident in the original operational taxonomic units (OTUs) —Lactobacillus, Enterococcus, Faecalibacterium, Ruminococcaceae UBA1819, Veilllonella, and Butyrivibrio,” the team says.
Of the six associations, the first four have been reported to be associated with RA, the study says and Ruminococcaceae were associated with RA Polygenic Risk Score (PRS) in the TwinsUK cohort.
According to the team, Butyrivibrio has not yet been associated with RA, but is a physiologically interesting taxa associated with the production of short chain fatty acid and host metabolism.
Source: Lancet Rheumatology
Published online: doi.org/10.1016/S2665-9913(20)30064-3
“Associations between gut microbiota and genetic risk for rheumatoid arthritis in the absence of disease: a cross-sectional study.”
Authors: Philippa Wells et al.