Respiratory Tract Infections (RTIs) affect one’s sinuses, throat, airways, and/or lungs. RTIs are a persistent and costly public health problem that even before COVID-19 pandemic were among the primary causes of death worldwide. The COVID-19 pandemic has only enhanced the problem. We know that the consequences are devastating and present an unprecedented challenge to public health, economy, and society.
Since 2020, COVID-19 has been the main RTI of concern, having caused almost 500 million infections and over 6 million deaths by March 2022 [9], and having extremely affected everyone’s lives. However, COVID-19 is not the only relevant RTI. Influenza alone infects up to 20% of the world’s population each year [13]. Another respiratory virus of great concern for young children is the Respiratory Syncytial Virus (RSV), responsible for the largest number of viral bronchiolitis in infants worldwide, and the main cause for hospitalization in this population group. The COVID-19 pandemic drastically changed the epidemiology of viral RTIs, including that of RSV. RSV infections virtually disappeared in 2020, only to re-emerge the following year stronger than before. In 2021 and 2022, the estimated incidence of RSV hospitalizations among 1-year-old children almost doubled compared to pre-COVID-19 incidence figures [10]. Pre-clinical data has shown CRL 1505 to protect against viral RTIs, and in particular RSV and influenza.
Some virologists have hypothesized that the lockdowns of 2020 meant infants and expectant mothers were not exposed to RSV that year, and therefore did not generate immunity. The relaxing of lockdown measures meant children were immunologically unprepared to fight the virus, resulting in higher numbers of hospitalizations than previously. In this context, boosting the immune system via probiotics to prevent RTIs seems an appealing strategy to lower the risk of RSV infections, precisely what CRL 1505 is thought to do.
A hidden threat of RTIs is the heavy use of antibiotics associated with these diseases. Despite most RTIs being viral in nature, up to 75% of antibiotics prescribed in high-income countries are to treat this kind of pathology [8]. This does not only impact the children receiving the antibiotic therapy but adds to the epidemiological problem of antibiotic resistance.
How can probiotics help
Probiotics play a role in the prophylaxis and management of several diseases and their side effects. The mechanisms by which probiotics exert these effects are several and still under study. Health benefits can arise indirectly, through the modulation of the gut microbiota that can in turn impact our health, or directly, through the stimulation of our immune system for example. Examples of direct interaction include the production of metabolites that inhibit pathogens in the gut (bacteriocins, organic acids, etc.), or the presence of cellular structures in the probiotic that can be recognized by our immune system and promote anti-inflammatory processes (i.e.: peptidoglycans), detoxification of some compounds, to name a few. Indirect health benefits on the other hand, can arise from metabolites produced by probiotics that can, in turn, be metabolized by our gut microbiota into health-promoting compounds; a clear example is acetate produced by bifidobacteria that can be converted into butyrate by some intestinal symbionts [11].
Today, the importance of probiotics and our microbiota in the context of viral infections is also of great importance, and the mechanisms of action underlined against general viral infections are also relevant for viruses such as SARS COV-2 and RSV, but need to be further explored.
Altered intestinal microbiomes have been described in COVID-19 patients: this can occur due to the disease itself which in some individuals causes diarrhea, or to the fact that most hospitalized COVID-19 patients (58–95%) are co-administered with antibiotics to prevent ventilator-associated pneumonia (VAP) and secondary bacterial infections. Thus, apt probiotic strains may help treat COVID-19-associated diarrhea and rebalance the patient's gut microbiota.
Probiotics may modulate the immune response of virally infected patients. The interplay between bacteria, viruses and host physiology is complex, and there is still a lot to be learnt. But what we know is that probiotic organisms can contribute to the host’s defense against viral pathogens in three main ways: i) enhanced mucosal barrier function that prevents viral invasion of the mucosae, ii) secretion of antiviral antimicrobial peptides, such as bacteriocins, and iii) modulation of the antiviral innate and adaptive immune response. Some probiotic strains have been shown to stimulate lung mucosal defenses for example, even if taken orally, due to their ability to trigger the innate immune responses both at local and systemic levels. In this way, once a bacterial or viral infection occurs, the host is ready to fight and keep the infection at bay.
Lacticaseibacillus rhamnosus CRL 1505 is a probiotic strain isolated from goat milk and widely studied in over 40 peer-reviewed publications for its ability to prime the immune system helping it to clear infections faster.
Clinical and pre-clinical evidence on CRL 1505
A randomized, double-blind, placebo-controlled trial with 298 pre-school children (2-5 years old) that consumed CRL 1505 (0,1 billion CFU/day) or a placebo 5 days/week for 6 months showed that children in the probiotic group had a significantly lower number of infections during the study period (Figure 1)[1]. CRL 1505 intake lowered the incidence of upper respiratory tract infections, pharyngitis, tonsillitis, and acute diarrhea. Additionally, kids in the probiotic group used fewer antibiotics and showed improved mucosal immunity as revealed by the levels of IgA in saliva (Figure 2).
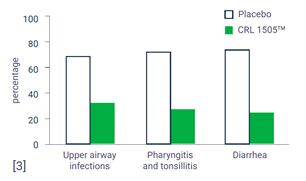
Figure 1: Effects of probiotic CRL1505TM on the incidence of common infectious diseases in pre-school children.
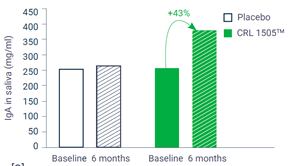
Figure 2: Effects of probiotic CRL1505TM on saliva IgA levels in pre-school children.
Pre-clinical studies evidenced that CRL 1505 can generate an earlier immune response to viral challenges with Influenza Virus or RSV, and to reduce lung damage [2-3]. The mechanisms of action of CRL 1505 include increased basal levels, key activators of the immune system, and of the anti-inflammatory cytokine interleukin 10 (IL-10). These modulations allow the immune system to be ready to tackle RTIs when one becomes in contact with the virus [5].
One of the key elements identified in CRL 1505 interaction with the host is its heat-stable peptidoglycan (PG05), which has proven to have a strain-specific immunomodulatory activity. PG05 significantly increases specific antibodies production and the number of alveolar macrophages. These cells, during viral and bacterial infections, play a key role in the beneficial modulation of the respiratory innate immune response [6-7].
- Villena J, Salva S, Núñez M, Corzo J, Tolaba R, Faedda J, Font G, Alvarez S. (2012). Probiotics for everyone! The novel immunobiotic Lactobacillus rhamnosus CRL1505 and the beginning of social probiotic programs in Argentina. International Journal of Biotechnology for Wellness Industries. 1: 189-198.
- Chiba E, Tomosada Y, Vizoso-Pinto MG, Salva S, Takahashi T, Tsukida K, Kitazawa H, Alvarez S, Villena J. (2013). Immunobiotic Lactobacillus rhamnosus improves resistance of infant mice against respiratory syncytial virus infection. International Immunopharmacology 17: 373-382.
- Zelaya H, Tsukida K, Chiba E, Marranzino G, Alvarez S, Kitazawa H, Agüero G, Villena J. (2014). Immunobiotic lactobacilli reduce viral-associated pulmonary damage through the modulation of inflammation–coagulation interactions. International Immunopharmacology 19: 161-173.
- Tomosada Y, Chiba E, Zelaya H, Takahashi T, Tsukida K, Kitazawa H, Alvarez S, Villena J. (2013). Nasally administered Lactobacillus rhamnosus strains differentially modulate respiratory antiviral immune responses and induce protection against respiratory syncytial virus infection. BMC Immunology, 14: 40.
- Salva S, et al. (2010). Immunomodulatory activity of Lactobacillus rhamnosus strains isolated from goat milk: Impact on intestinal and respiratory infections. Int J Food Microbiol 141(1-2): 82-9.
- Clua P, et al. (2020) The Role of Alveolar Macrophages in the Improved Protection against Respiratory Syncytial Virus and Pneumococcal Superinfection Induced by the Peptidoglycan of Lactobacillus rhamnosus CRL1505. Cells 9;9(7):1653.
- Kolling Y, et al. (2018). Are the immunomodulatory properties of Lactobacillus rhamnosus CRL1505 peptidoglycan common for all Lactobacilli during respiratory infection in malnourished mice? PLoS One. 13(3):e0194034.
- Wang Y et al. Probiotics for prevention and treatment of respiratory tract infections in children: A systematic review and meta-analysis of randomized controlled trials. 2016 Medicine (Baltimore) 95(31):e4509.
- https://covid19.who.int/
- Zheng Z, Pitzer VE, Shapiro ED, Bont LJ, Weinberger DM. Estimation of the timing and intensity of reemergence of respiratory syncytial virus following the COVID-19 pandemic in the US. JAMA Netw Open. Published online December 1, 2021. doi:10.1001/jamanetworkopen.2021.41779
- Klaenhammer, T., Kleerebezem, M., Kopp, M. et al. The impact of probiotics and prebiotics on the immune system. Nat Rev Immunol 12, 728–734 (2012).
- Hernández-Rivas L, Pedraz T, Calvo C, Juan IS, José Mellado M, Robustillo A. Respiratory syncytial virus outbreak DURING THE COVID-19 PANDEMIC. How has it changed? Enferm Infecc Microbiol Clin. 2021 Epub ahead of print.
- Clayville LR. Influenza update: a review of currently available vaccines. P T. 2011;36(10):659-684.




