A new report from Frost & Sullivan has found that higher intakes of calcium and vitamin D for a target population of over 55s could save €19.8 billion in healthcare costs over five years, and provide a return of €3.47 in savings for every €1 spent on supplements or fortification.
The new report – commissioned by Food Supplements Europe but carried out independently – provides analysis of the costs and savings that the use of a 1,000 mg calcium plus 15 µg vitamin D supplements could bring to European Union Member States when targeted to the ‘at risk’ over 55’s population, where there is an increased possibility of fractures and associated costly medical treatment.
It noted that recent evidence has shown the combination of calcium and vitamin D can reduce the incidence of osteoporosis-related fractures by around 15% - with an EFSA approved risk reduction claim on the loss of bone mineral density, “which may contribute to a reduction in the risk of osteoporotic bone fracture” relating to an intake of at least 1200 mg of calcium and 800 I.U. [20 µg/day] of vitamin D from all sources.
“Over several decades, a significant amount of clinical research has been conducted showing that the daily use of calcium and vitamin D food supplements is highly correlated to a lower risk of experiencing an osteoporosis-attributed fracture,” said Ingrid Atteryd, chair of Food Supplements Europe. “This new analysis, for the first time, demonstrates that more widespread supplementation with these nutrients could also save many billions of euros in avoidable healthcare costs.”
“The EU’s population is ageing and without taking action the number of bone fractures attributed to osteoporosis will almost certainly rise. As such it has never been more important to leverage the substantiated benefits of calcium and vitamin D to help minimise the financial burden of this disease on healthcare systems across Europe,” she added.
The new Frost & Sullivan study is the second in-depth analysis commissioned by Food Supplements Europe to examine the positive impact of supplementation on EU healthcare costs. Last year, its first report highlighted possible €12.9 billion a year savings on spending for cardiovascular disease through more widespread consumption of omega 3 EPA+DHA supplements by people aged 55 or over.
The figures behind the facts
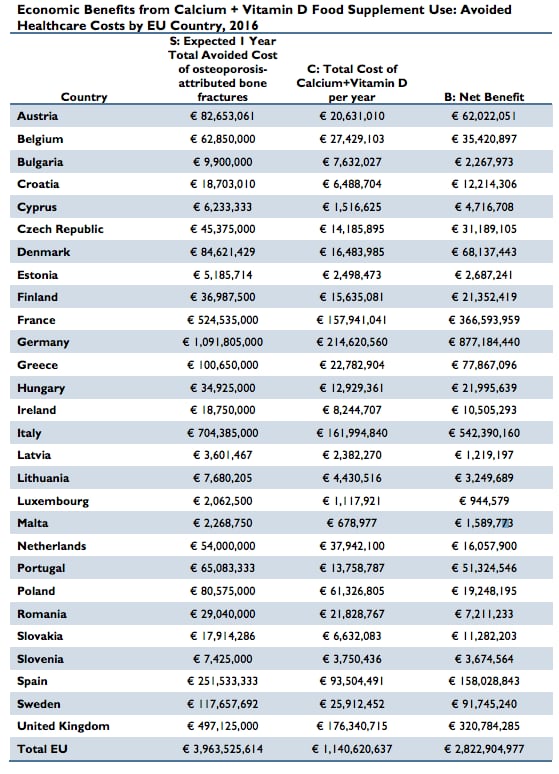
The headline figure of a total potential savings of € 3.96 billion per year is calculated based on the sum total of Frost & Sullivan analysis data that worked out each EU country’s potential cost savings from avoided bone fractures among the target population of adult’s age 55 and older.
The total economic burden of osteoporosis-related bone fractures in the EU is calculated to be €26.4 billion per year – averaging at €21,231 per event for the 1.2 million fractures that happen every year.
Over five years, the total cost of fractures in the over 55s attributed to osteoporosis will amount to €132 billion – with a potential saving of almost €20 billion of healthcare costs calcium and vitamin D prevention, the report said.
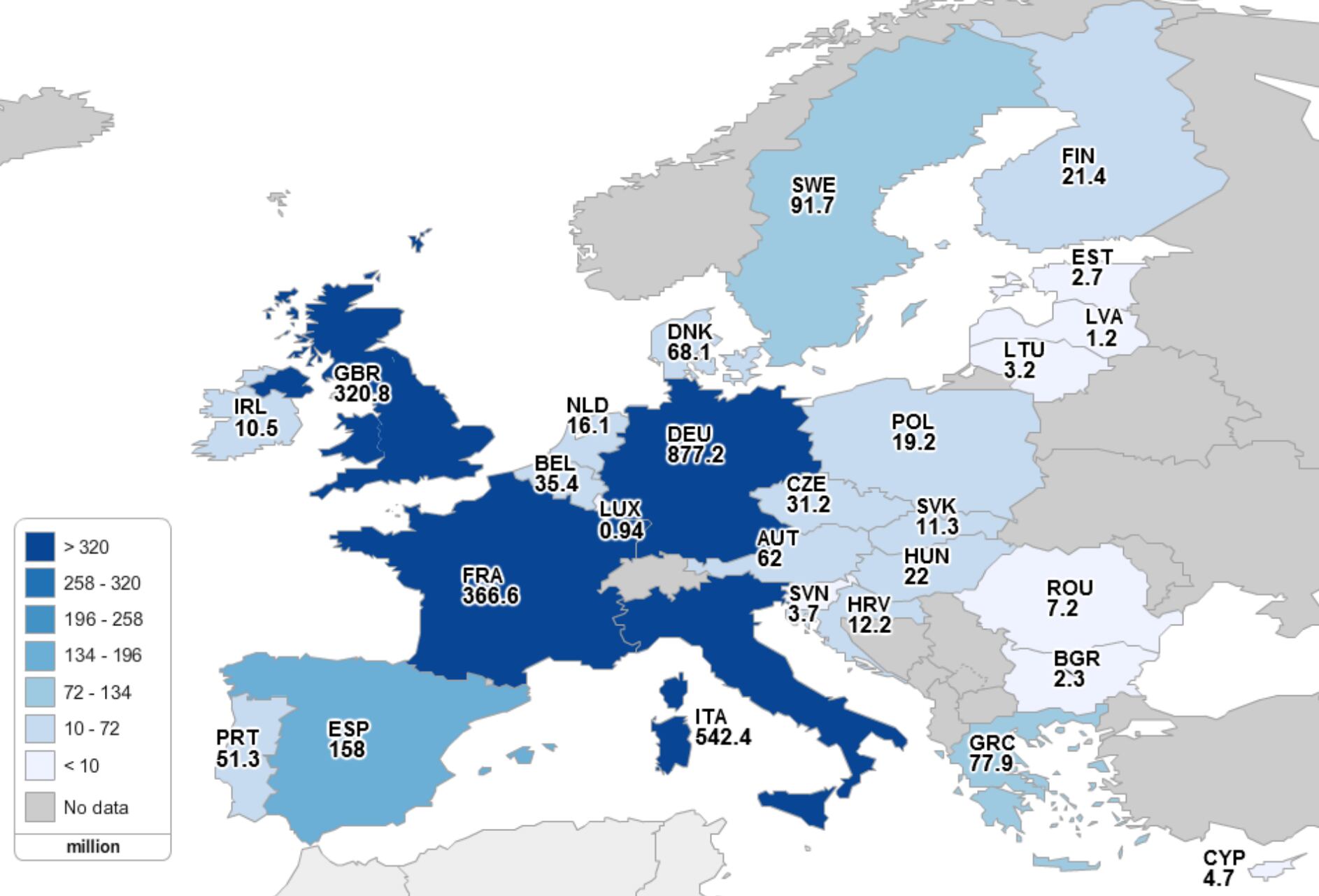
According to the country-by-country data, Luxembourg has the lowest potential savings (€2.1 million per year) followed by Malta (€2.3 million per year). Meanwhile Germany has the highest potential savings of €1.09 bn.
“Overall, the five largest EU countries (France, Germany, Italy, Spain, and the UK) combined can expect potential cost savings in excess of €200 million per country per year if the entire target population of adults age 55 and older used calcium and vitamin D on a daily basis,” the report states.
“Thus, a targeted calcium + vitamin D supplement regimen is recommended as a means to help control rising societal healthcare costs and as a means for high-risk individuals to minimise the chance of having to deal with potentially detrimental disease-attributed events.”
Cost-benefit
Speaking with NutraIngredients before the release of the report, Patrick Coppens, director of regulatory and scientific affairs at Food Supplements Europe said that even when the additional costs of supplementation or fortification are factored in to the analysis, a net saving of € 2.82 billion can still be achieved within the EU.
He added that while it is known that adequate intake of calcium and vitamin D in younger life stages is important in laying foundations for the prevention of osteoporotic fractures, the data used in the report focuses on supplementation in later life stages – which can only counteract or slow down a decline of the status that has been built up in earlier ages.
“The age cohort threshold of 55 and older was adopted for this case study in order to provide a conservative assessment of the health and economic benefits to current and potential users,” said the report.
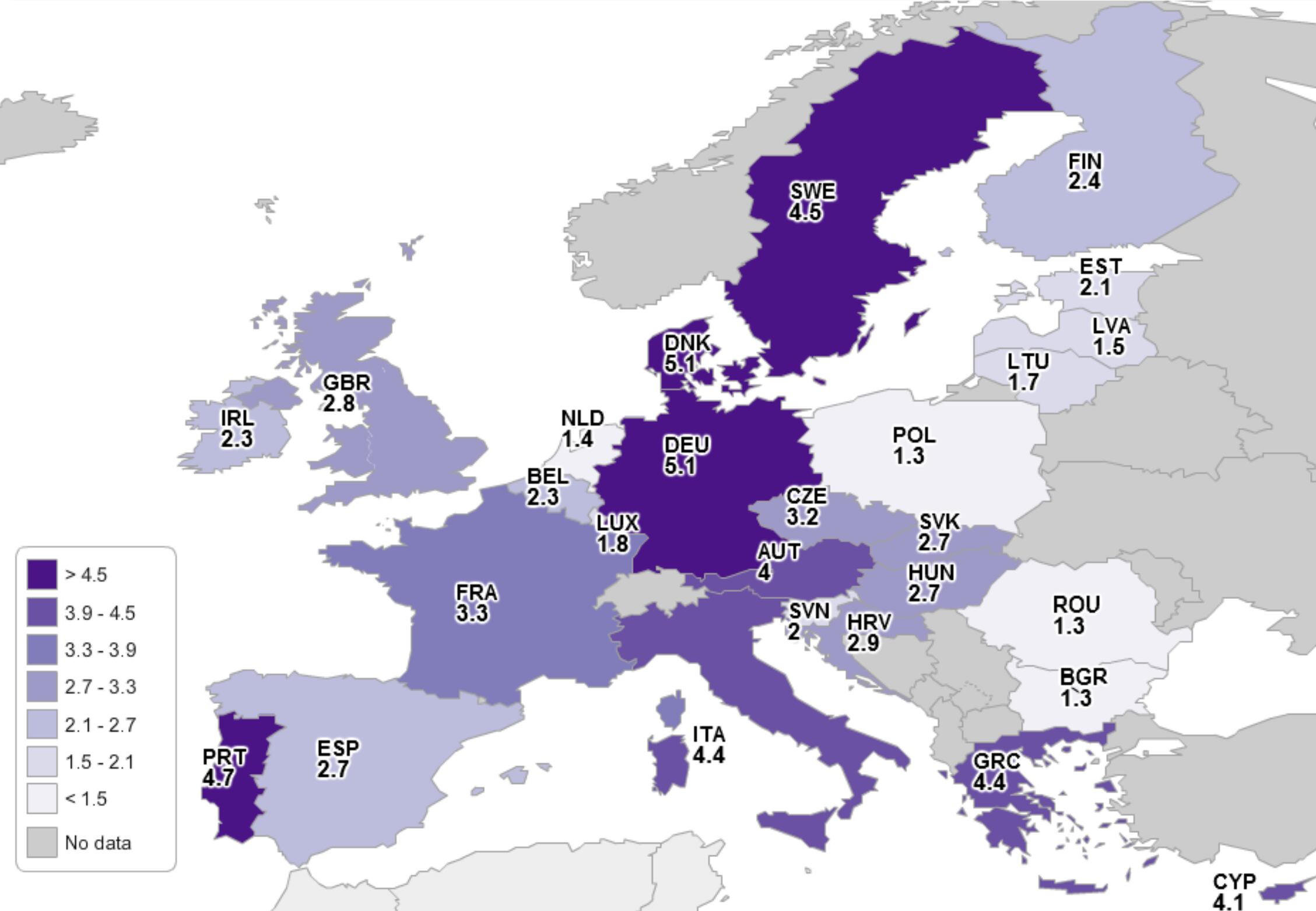
On average, the report finds that for every € 1.00 spent on a calcium + vitamin D food supplement, there would be a certainty equivalent return of €3.47 to users and society as a whole in the form of avoided healthcare expenditures attributed to osteoporosis.
In a country-by-country analysis of these benefits, Denmark, Germany and Sweden come with the biggest returns, while Poland, Romania and the Netherlands stand the least to gain (with a return of between €1.3 and €1.4 savings per €1 spent).
“There would be a significant portion of cost savings to the primary payers of healthcare costs, which include governments and insurance companies,” said the report. “In fact, all 28 EU countries have benefit cost ratios greater than € 1.00 which is an indication of cost effectiveness.”
INFOGRAPHIC

