A study by Canadian researchers at the University of Alberta found that caesarean birth and prolonged labor impact infant gut bacteria, leading to a higher risk of childhood obesity and allergies.
The study
The team collected stool samples from the diapers of 1,667 infants who are part of CHILD, a national birth cohort study that aims to discover the root causes of allergies, asthma, obesity and other chronic diseases. The cohort involves about 3,500 Canadian children from before birth to adolescence.
Using data from the CHILD cohort, the research team examined directional relationships between birth details, baby's gut microbiome, breastfeeding, metabolites, immune function, childhood BMI and atopy in 1667 infants. These factors were analyzed at three months and again at one year. Health outcomes were also noted at ages one and three.
Findings
The research team was able to link factors such as C-section delivery and prolonged labor to changes in the gut microbes of infants.
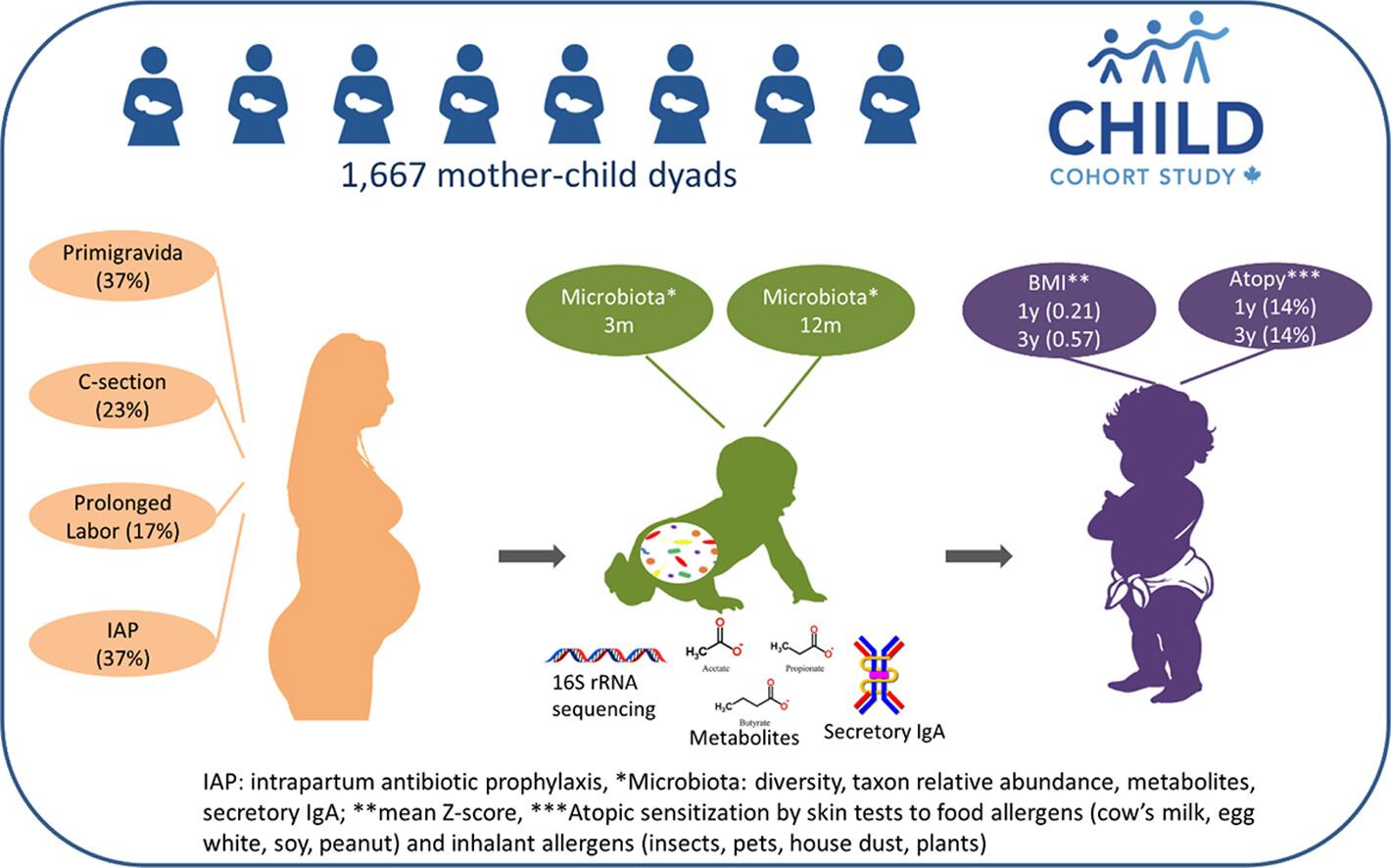
The study showed that infants born by C-section were more likely to have a high body-mass index score at ages one and three. From there, the scientists determined the pathways from these alterations may lead to an increased risk of allergies and obesity later in childhood.
Looking at the baby’s microbiome profiles at three months of age, they found that an altered ratio of Enterobacteriaceae and Bacteroidaceae (E/B) bacteria were the dominant routes to becoming overweight.
At 12 months of age, a higher E/B ratio and colonization with Clostridioides difficile (C. difficile) were found to be the main pathways leading to allergic sensitization.
“Following both cesarean birth, and prolonged labour with a first pregnancy, a higher Enterobacteriaceae/Bacteroidaceae (E/B) ratio at 3 months was the dominant path to overweight; higher E/B ratios and Clostridiodes difficile colonization at 12 months were the main pathway to atopic sensitization. Depletion of Bifidobacterium following prolonged labour was a secondary pathway to overweight. Influenced by C. difficile colonization at 3 months, metabolites propionate and formate were secondary pathways to child outcomes, with a key finding that formate was at the intersection of several paths,” the authors noted.
Senior author Anita Kozyrskyj, a CHILD investigator and professor in the Faculty of Medicine & Dentistry at the University of Alberta, said the takeaway from the study is that exposures at birth can trigger multiple and common gut microbial pathways leading to child overweight and allergic sensitization.
"Understanding how disruptions to the gut microbiome affect health in later childhood means we may have several options for effective interventions to prevent these chronic conditions before they become established,” she said. "We may want to take steps to avoid unnecessary cesarean section deliveries, and possibly consider postnatal microbiota solutions that may help to prevent these two conditions."
Postnatal microbiota solutions
One such postnatal microbiota solution is an orally-delivered maternal fecal microbiota transplantation (FMT).
In a separate study, researchers from the University of Helsinki demonstrated this method can restore the intestinal microbiota development in babies following a c-section.
"This simple procedure can normalize gut microbiota colonization and development in C-section born infants, which will likely contribute to reduced risk of developing chronic diseases that abnormal gut microbiota may confer," said Dr. Otto Helve MD, specialist in pediatric infectious diseases and shared first author of the study.
Clinical trial
The researchers recruited 17 mothers who were scheduled to undergo elective C-sections. Three weeks before delivery, the team collected stool and blood samples from the mothers to screen for infectious pathogens, including HIV, hepatitis, Clostridium difficile, Helicobacter pylori, norovirus, drug-resistant bacteria, group B streptococcus, and a long list of others. Based on the results of the screening, seven of the mothers were selected to continue with the procedure.
Once the babies were born, each was given a dose of a few million cells of live fecal bacteria in their first milk feeding. Their health was monitored for two days in the maternity ward with follow-up visits at four weeks and three months. No adverse health effects were reported.
Stool samples from the babies were also collected after two days, then each week for four weeks and then again at 12 weeks.
Key findings
The samples were analyzed along with control samples collected from 29 vaginally-born babies and 18 untreated cesarean-delivered babies. The findings showed that the while the gut microbiota of the treated and vaginally-born babies differed in the early days, after a week they were significantly more similar to each other, and both were distinct from the microbiotas of untreated C-section babies.
"The gut microbiota of the FMT-treated infants became very quickly similar to that of vaginally born infants. It did not resemble that of the untreated C-section born infants, showing that the treatment was effective in restoring normal microbiota development," noted Dr. Katri Korpela, shared first author on the study.
When comparing untreated C-section babies with those delivered vaginally or FMT-treated, researchers observed that the control infants had a lower amount of commensal Bacteroides and Bifidobacteria species, but a higher abundance of more pathogenic taxa.
Proof-of-concept
“This proof-of-concept study demonstrates that the intestinal microbiota of infants born by C-section can be postnatally restored by maternal FMT and provides further support for the natural transfer of gut microbiota from mother to infant,” said microbiologist and immunologist Willem de Vos of the University of Helsinki and Wageningen University, who led the research.
While researchers note that larger and longer-term studies are needed, the study does provide a blueprint for the procedure and a further understanding of the microbe restoration process in infants born via C-section.
Source: Gastroenterology
2020, doi: 10.1053/j.gastro.2020.08.053
“From birth to overweight and atopic disease: multiple and common pathways of the infant gut microbiome”
Authors: K. Vu et al.
Source: Cell
2020, doi:10.1016/j.cell.2020.08.047
“Maternal fecal microbiota transplantation in cesarean-born infants rapidly restores normal gut microbial development: a proof-of-concept study”
Authors: K. Korpela et al.