Juan Pablo Stefanolo, MD, a lead author on the study and a physician with the Neurogastroenterology and Motility section, Hospital de Clínicas José de San Martín, Buenos Aires University, Argentina, presented data from the study, "Gut-brain axis and irritable bowel syndrome during SARS-CoV-2 pandemic. A survey-based study" at the virtual event yesterday (May 23).
He explained pandemic lockdown orders in Argentina created a unique opportunity for researchers to study the impact of pandemic stressors and reduced social interaction on 129 IBS patients whose pre-pandemic data had already been collected through an earlier research project.
The patients were re-assessed during the lockdown with the same online survey that included multiple validated measures of IBS severity, anxiety and depression, along with questions about co-occurring illnesses, including heartburn, regurgitation, indigestion, chronic fatigue, fibromyalgia and nonmigraine headaches.
The researchers' main hypotheses was that these patients were going to be worse because of pressure and stress due to COVID-19.
Instead, during the lockdown in Argentina, the number of patients experiencing severe IBS fell sharply from 65 to 39. The mean Irritable Bowel Syndrome Severity Scale score for the group also fell 66 points, from 278 to 212 on a 500-point scale. IBS symptoms of pain, distention, stool consistency, anxiety, somatization, fibromyalgia and chronic fatigue symptoms all improved during the lockdown.
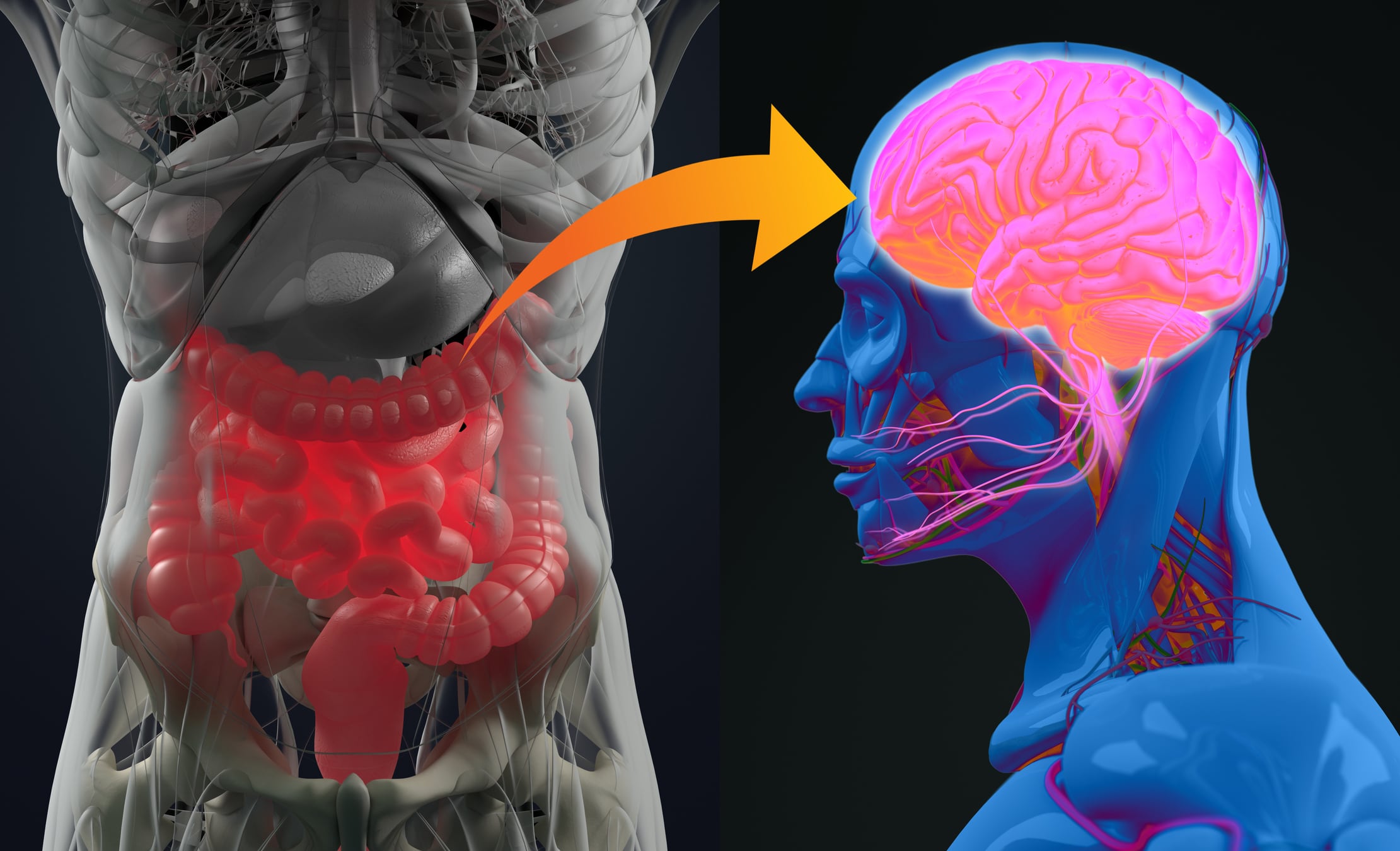
Patients with functional gastrointestinal disorders experience symptoms even though no structural or biochemical abnormalities are present. The gut-brain connection refers to the role of stress and psychological difficulties in triggering debilitating gut-related symptoms. Headache, heartburn and regurgitation - all outside the category of functional disorders - became worse during the study, which the authors hypothesise is likely due to the increase in weight that nearly 60 percent of patients reported.
"We think the results have something to do with people staying at home. They were not exposed to outside stress, and at home they were able to avoid food triggers," Dr. Stefanolo explains.
"Our results reinforce the concept that IBS, or functional gastrointestinal disorders, have a connection to psychosocial factors, as well as food and other factors... The gut-brain axis has a lot of facets."