The new review was published this week in the journal Gastroenterology Report. It was the work of a team led by researchers associated with institutions in Australia, Brazil and CalTech in California.
Accumulating evidence for connection
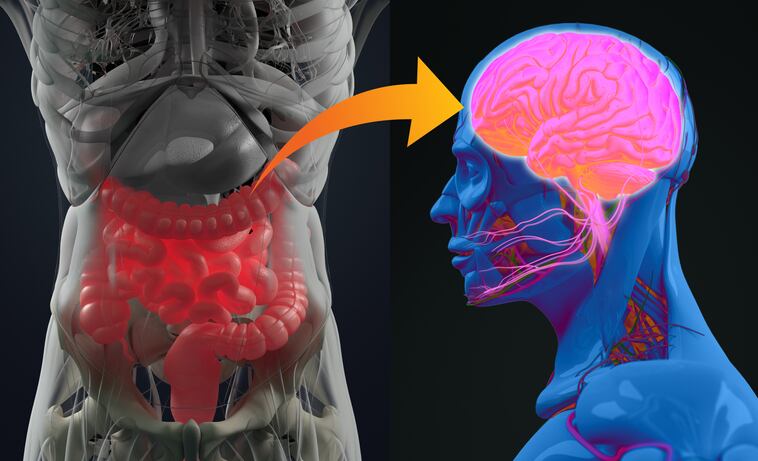
The authors said evidence is accumulating that conditions in the gut play a key role in the development and progression of neurodegenerative disorders such as Alzheimer’s disease, ALS, Huntington’s disease, multiple sclerosis and Parkinson’s disease. These conditions all have life changing and in most cases fatal implications, and few good pharmaceutical treatments exist.
Just as the neurodegenerative conditions mentioned by the researchers are complex, so too is the potential pathways by which the gut and the brain can interact. Recent research has focused on transmission of signals via the vagus nerve as well as the secretion of hormones and neurotransmitters in the gut.
But other pathways by which conditions in the in gut could influence the brain exist. These include the production of short chain fatty acids by gut microbes (i.e., butyrate, propionate, and acetate) as well as the function of the enteric nervous system (ENS), a diffuse system that runs in parallel with the vagus nerve. In addition, the immune system, which is intimately linked with conditions in the gut, also figures into neurodegenerative disorders.
One of the common threads among all of these conditions is inflammation, both systemic and specifically affecting the nervous system, the authors said. This is linked to a host of external and internal factors including genetics, environmental stimuli and diet and lifestyle choices. But they said there is growing evidence that the gut microbiome can act as a filtering agent for these stimuli, either blunting or exacerbating their effects.
“There is evidence that potential key factors, including aging, diet, lifestyle choices, and exposure to xenobiotics, can influence the likelihood of developing neurodegenerative disorders. Interestingly, the gut microbiota is capable of interacting with these factors, acting as an intermediate element between the host and the environment in the etiology of neurodegenerative disorders,” they said.
“Due to particularities of each neurodegenerative disease mentioned, their courses, gravities, and roles of inflammation can vary; however, there is a convergence in the mechanisms responsible for the inflammatory process in these diseases. Furthermore, a tight connection between the gut microbiota and inflammation has been widely demonstrated,” they added.
The mechanisms of action remain to be elucidated, the authors said. There is some limited evidence for higher production of SFCAs and lower inflammation. There is slightly more data, they said, connecting tryptophan metabolism and neurodegenerative conditions.
Shifting the gut in the right direction
Another key element of equation is the generally negative changes in the gut during the aging process. Aging is also a key risk factor for most of the neurodegenerative conditions mentioned with the exception of MS, which rarely appears after 60 years of age. Do these two things — a degraded gut with age and a higher risk of developing a neurodegenerative condition — happen in parallel? Or does the first influence the second? The jury’s out, the researchers said, but some preliminary research done in animal models seems to suggest a link, they said.
Diet and exercise are the two most obvious and best supported ways to shift the gut in a positive direction, the authors said. Probiotics, prebiotics or synbiotic formulations (the authors refer to these as ‘symbiotics’) have some good data behind them in regard to their ability to positively modify conditions in the gut as well. They said making a blanket statement about their effects is hampered by the many different ingredients involved and a lack of consensus on dosages and treatment length.
“Despite huge research efforts, the cause of the various neurodegenerative disorders is mostly unknown with genetic and environmental contributors. As noted in this review, the gut microbiota may act as an intermediate factor between the host and the environment, affecting key aspects in the neurodegeneration process such as inflammation and protein homeostasis. However, a causal role for the gut microbiota in neurodegeneration is missing. Many of these challenges are rooted in the limitation of translating animal findings to humans. Several animal models have been used to study neurodegenerative conditions, yet they fail to capture the complexity of multifactorial disorders,” the authors wrote.
“A better understanding of the role of the gut microbiota in neurodegenerative disorders is essential and may lead to the discovery of new therapeutical targets and/or disease-modifying strategies,” they concluded.
Source: Gastroenterology Report
doi.org/10.1093/gastro/goac017
Convergent pathways of the gut microbiota–brain axis and neurodegenerative disorders
Authors: Gubert C, Gasparotto J, Morais LH