One of the characteristics of COVID-19 disease is the exacerbated inflammatory response that occurs in a second phase of the disease. Thus, one of the main investigations that has been carried out around the world is to dissect how the infection occurs in each tissue and systems and how that tissue reacts to the presence of this infection.
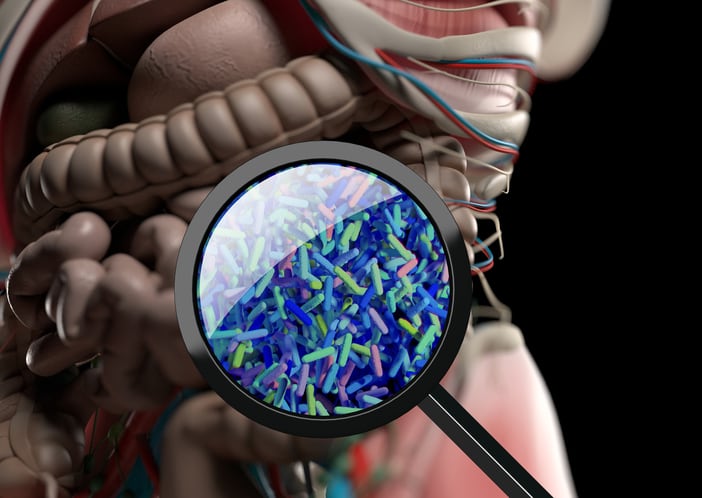
Up to 50% of COVID-19 patients experience gastrointestinal symptoms such as diarrhea, vomiting, and abdominal pain, with symptoms detected in 17.6% of severe cases. This is partly associated with viral entry into intestinal cells resulting in alterations to their normal functions. In addition, recent studies point to major changes in COVID patients’ gut microbiota, including a decrease in levels of bacteria that secrete short-chain fatty acids (SCFAs).
Thus, there is evidence that the presence and infection of COVID-19 in the gut is associated with changes in microbiota including the reduction in SCFAs-producing bacteria. However, previous studies have not addressed whether this effect on SCFAs is relevant for the infection.
Researchers from the University of Campinas (UNICAMP), in Brazil, conducted the current study with the aim to confirm whether SCFAs directly affect the infection of intestinal cells by SARS-CoV-2.
The in-vitro study, funded by the São Paulo Research Foundation (FAPESP), saw healthy colon tissue and epithelial cells infected with SARS-CoV-2 before being subjected to a battery of tests.
They found that bacteria and other microorganisms produced in the gut during fermentation of insoluble fibre did not affect the ability of the virus to thrive. However, they did find this fermentation reduced the expression of a gene that plays a key role in viral cell entry and a cytokine receptor that favours inflammation.
Raquel Franco Leal, a professor at UNICAMP’s School of Medical Sciences and co-principal investigator for the study, said: “Treated intestinal biopsy samples displayed a significant decrease in expression of the gene DDX58 - an innate immune system receptor that detects viral nucleic acids and activates a signalling cascade that results in production of pro-inflammatory cytokines - and the interferon-lambda receptor, which mediates anti-viral activity. There was also a decrease in expression of the protein TMPRSS2, which is important to viral cell entry.”
Protection against inflammation
The researchers took colon tissue samples from 11 patients without COVID-19. They also tested epithelial cells that line the intestines and are in close contact with gut microbiota. Tissue and cell samples were infected with SARS-CoV-2 in IB-UNICAMP’s Laboratory of Emerging Virus Studies (LEVE), a Biosafety Level III (BSL-3) facility.
The tissues and cells were treated with a mixture of acetate, propionate and butyrate, compounds produced by gut microbiota metabolisation of SCFAs present in dietary fibre. The treatment did not alter viral load in colon biopsies or cells, nor were there any changes in cell wall permeability and integrity.
Patrícia Brito Rodrigues, who has a doctoral scholarship from FAPESP and was joint first author of the article, said: “That doesn’t exclude the possibility of significant action by SCFAs on infection by SARS-CoV-2. The anti-viral effects could depend on interaction with other cells in the organism.
“We’ll continue our investigation in animal models since the action of these compounds on the infection could depend on a more complete system than the samples we used in vitro [isolated cells and tissues].”
Other tests involving non-treated infected biopsy samples showed an increase in expression of the gene DDX58, which encodes an important viral receptor, and of interferon-beta (IFN-beta), a pro-inflammatory molecule that participates in the cytokine storm associated with severe cases of COVID-19.
“Alterations in genes associated with virus recognition and response during intestinal infection may be relevant to the onset of the inflammatory chain,” Leal said. “In this context, it will be important to deepen the analysis of the effects of SCFAs with these parameters, as this could be significant in severe stages of the disease.”
Gut-COVID axis
Gut microbiota composition has previously been described as being associated with the severity of COVID-19 and the risk of on-going symptoms.
Published in 'Gut', a recent observational study found associations between gut microbiota composition and levels of cytokines and inflammatory markers in patients with COVID-19. The researchers conclude that the gut microbiome is involved in COVID-19 severity possibly via modulating host immune responses.
The researchers also suggest the gut microbiota dysbiosis after disease resolution could contribute to persistent symptoms, aka 'long COVID', highlighting a need to understand how gut microorganisms are involved in inflammation and COVID-19.
Professor Tim Spector, who works as a genetic epidemiologist at King's College London, has been a key thought leader in this space. Right at the beginning of the pandemic, he highlighted research that showed the gut microbiome’s role in the body’s immune response to infection as well as its role in preventing not only damage to lungs but also to other vital organs.
Writing in The Conversation, professor Spector said that whilst the finer details of gut microbiome and the immune system interactions are not fully understood, there may be a link between the microbiome makeup and inflammation – one of the immune response’s traits.
He also pointed out that gut bacteria produce many beneficial chemicals and also activate vitamin A in food, which helps to regulate the immune system.
Professor Spector also said that rather than take supplements, the food we eat has a big impact on the gut and the best way to increase microbiome diversity is by eating a wide range of high-fibre plant-based foods, such as those found in a Mediterranean diet.
Source: Gut Microbes
Pascoal. L. B., et al
"Microbiota-derived short-chain fatty acids do not interfere with SARS-CoV-2 infection of human colonic samples"