Globally, the number of people aged 60 years or over is expected to more than double by 2050, rising from 962 million in 2017 to 2.1 billion, according to the latest UN World Population Prospects report.
The 60+ population is growing faster than all younger age groups at around 3% each year and by 2100 there will be 3.1 billion globally. Persons aged 80 and over will also triple by 2050 to around 425 million.
According to the UN, Europe currently has the highest percentage of population aged 60 or over, with 25% falling into this demographic.
From a health standpoint, this population faces a number of age-related challenges, including cardiovascular disease (the leading cause of death worldwide); mobility issues from muscle and bone loss; cognitive decline; and diabetes, among others. And Peter van Dael, senior vice president for Nutrition Science and Advocacy at DSM, said it's very often malnutrition that creates the window to develop such non-communicable diseases and health problems.

“Quite a lot of us, despite the fact we probably eat enough, are not adequate in our nutritional status and that is clearly a challenge we face,” Van Dael told NutraIngredients.
“So, if you're inadequate you should have hundreds of a certain nutrient in your bloodstream – you don't have a deficiency but you don't operate ideally. If you combine that with a number of these deficiencies, you may start to develop non-communicable diseases and that is basically where hidden hunger is the leading entry point to develop, ultimately, a non-communicable disease.”
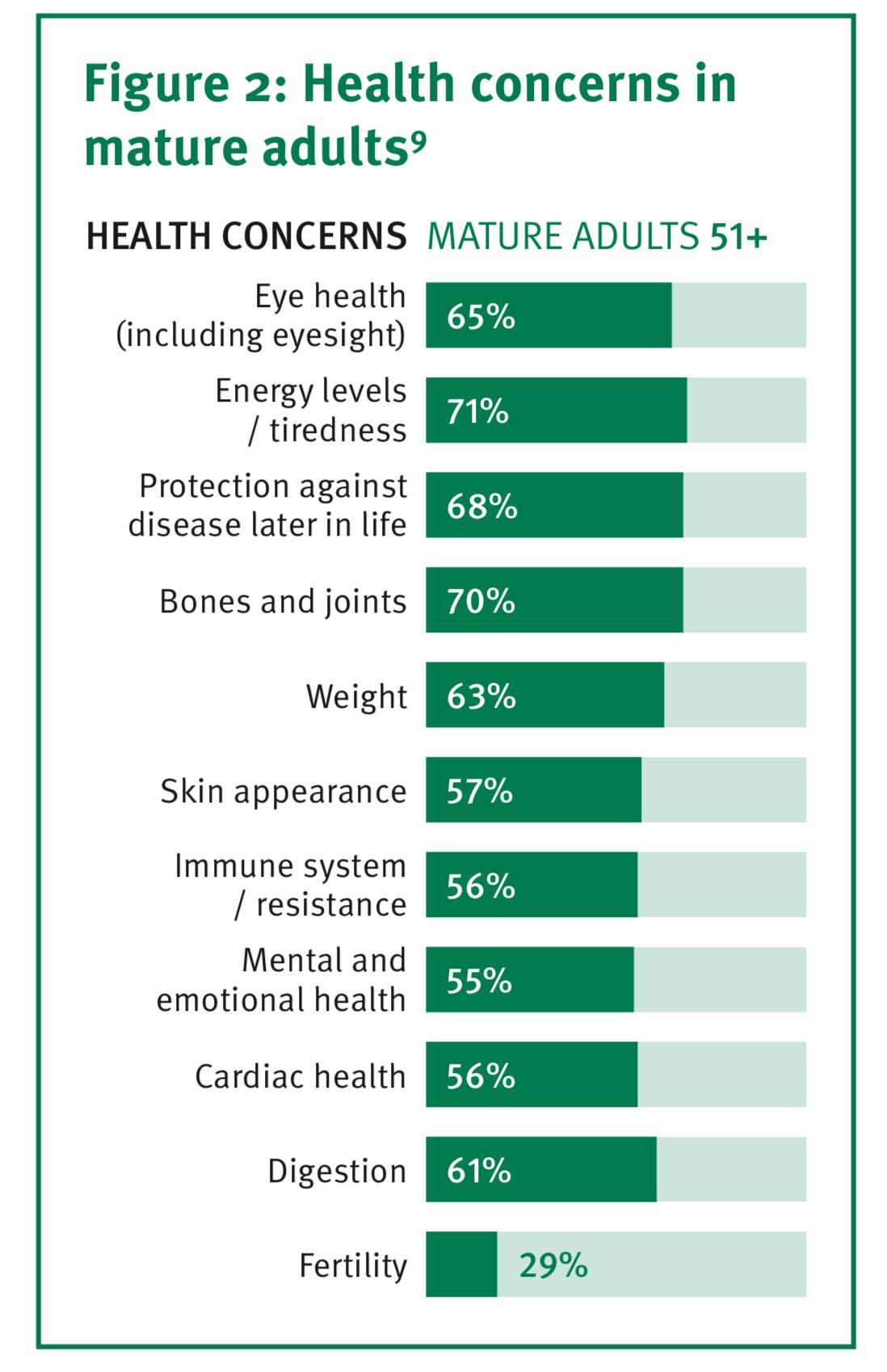
And, according to DSM's 2017 Global Health Concerns study, 67% of adults worldwide worry about the protection against disease later in life, with mature adults aged 51 and over specifically concerned about energy levels and bone and joint health.
'We really should not forget the value of adequate nutrition'
Van Dael said ensuring the ageing population has access to adequate nutrition to plug deficiencies and hidden hunger will be key in preventing the onset or worsening of numerous health conditions.
“If you ask me, we should indeed focus more on the positive role of adequate nutrition that can then play a role in well-being; in your healthy life; and in reducing the risk or prevention of some later-life healthy ageing disorder. I think we really should not forget the value of adequate nutrition, per se.”
Unfortunately, he said industry and research tends to focus too heavily on added benefits when the importance lies in essential nutrition to support good functioning – especially important in the elderly.
If someone is already optimal in vitamin D, for example, taking more will not provide additional benefits so, on paper, it could be considered there is no benefit to taking this nutrient. In this instance, Van Dael said “we actually destroy the story that this nutrient has an essential role in our body function”.
“...This is where I see research today is facing, quite often, a challenge. We say we need more data to prove benefits and I think we don't put enough efforts on communicating that nutrition has a key, essential role that is defined as a requirement.”
Nutrient status data needed
However, Van Dael said there is currently a lack of strong data on the true nutritional gaps in the elderly.
“Vitamin D is definitely one we can very consistently say is low (…) In general, vitamin levels are low in the ageing population – that's a general observation – and then also micronutrients are quite often lower. But, one of the things that is not always very good is do we have a good picture based on real data? No, we don't have a very good picture based on real data and that's a big challenge.”
Whilst there have been numerous assessments done on nutrients and deficiency levels in the elderly, he said there are few systematic reviews of the overall nutrient status in the elderly.
Considering this is a population that visits the doctor regularly, Van Dael said there is scope to collate data easily and track nutrient status to develop targeted nutritional plans.
“It might be something that health systems be more active on. We could have an insurance system that covers regular checkups and it could be that, for example, the yearly checkup should also make an assessment of the nutrient and vitamin status and then, in the end, recommend or reimburse supplementation if people were to be too low.”
“....Personalising nutrition for the elderly is probably a tool that we need to explore very much and then within that, there is definitely one thing that is critical and that is where governments or insurance companies need to jump in.”
Chewing over product development
Meanwhile, Van Dael said industry needs to stay focused on developing suitable products for this population - both supplements and fortified food and beverages.
“We eat foods, not nutrients,” he said. “Clearly, we need to have fortified foods if people only have a limited selection of food. Of course, a balanced diet is always best but we know that by ageing, and even in our lives as healthy adults, we can't always eat everything so then fortification of food will always remain important and is, for me, a key element. However, the moment you don't necessarily have access to the right food or have to take a bit of a higher dose at some point in time, then supplements are critical.”
The key to developing such products for the elderly, he said, remains appeal. “I think the organoleptic properties and the form in how they can be consumed is definitely superior to bioavailability. As a scientist, I would say bioavailability is more exciting however, if a person doesn't want to eat a highly-bioavailable food source, they're not going to eat it. You first need to sort out organoleptic issues – chew-ability and the appearance of the food needs to be pleasurable.”
Packaging is also important, he said, particularly in an ageing population that doesn't like to feel differentiated. “We should, as companies, produce things that are loved by the youngsters and elderly and something both want to buy. And that's the challenge.”

